Knee pain is one of the top reasons people visit an orthopaedic doctor in Indore. And it is easy to see why. The knee is the largest joint in the body, takes on enormous load every single day, and when something goes wrong inside it, even walking to the kitchen becomes a task.
What makes knee pain frustrating for most patients is that they do not know what is actually wrong. They live with it, take painkillers, rest for a few days, and assume it will sort itself out. Sometimes it does. More often, it does not – and what started as a manageable ache turns into something that needs a much more serious intervention than it would have required six months earlier.
Dr. Prince Uchadiya is a Gold Medalist orthopaedic surgeon in Indore with over 2,500 successful surgeries and more than 10 years of focused clinical practice. This article is built around how he actually approaches knee pain – from finding the right diagnosis to choosing the right treatment, and understanding when surgery is genuinely the answer versus when it is not.
Why Knee Pain in Indore Is No Longer Just an Older Person’s Problem
The average age of knee pain patients in Indore has dropped noticeably over the past decade. Younger patients – people in their 30s, sometimes even late 20s – are increasingly presenting with structural knee problems that would previously have been seen mostly in patients over 50. Several things are driving this shift.
Sedentary work is one of the biggest factors. Long hours sitting at a desk weaken the quadriceps and hip muscles that are supposed to absorb load on behalf of the knee joint. When those muscles are not doing their job, the joint takes all the stress directly – and it was not designed for that.
Bodyweight is another. Every extra kilogram of body weight adds roughly 4 kg of force on the knee with each step. For someone who is 10 kg overweight, that is 40 kg of additional pressure on the joint thousands of times a day. Combined with increasingly sedentary lifestyles, this is accelerating cartilage wear in people who are far too young for it.
Unregulated gym activity and weekend sport play a big role too. People who sit at desks all week and then play intense cricket, football, or badminton without warming up are tearing ACL ligaments and damaging meniscal tissue at rates that were uncommon a decade ago. Poor gym form – particularly heavy deep squats and lunges done without proper technique – adds to the toll.
And Vitamin D deficiency, which is extremely widespread across Indore and Central India, is weakening bone density in the background for years before any symptoms appear. The World Health Organization identifies musculoskeletal conditions, including knee osteoarthritis, as the leading cause of disability globally affecting over 1.7 billion people. India carries more than its share of that burden.
8 Causes of Knee Pain a Specialist in Indore Will Actually Look For
This is where most patient journeys go wrong. People get told they have “knee pain” and get a generic treatment plan. But knee pain is not one condition – it is a symptom of many very different conditions, each of which needs a different approach. Here is what Dr. Prince Uchadiya looks for:
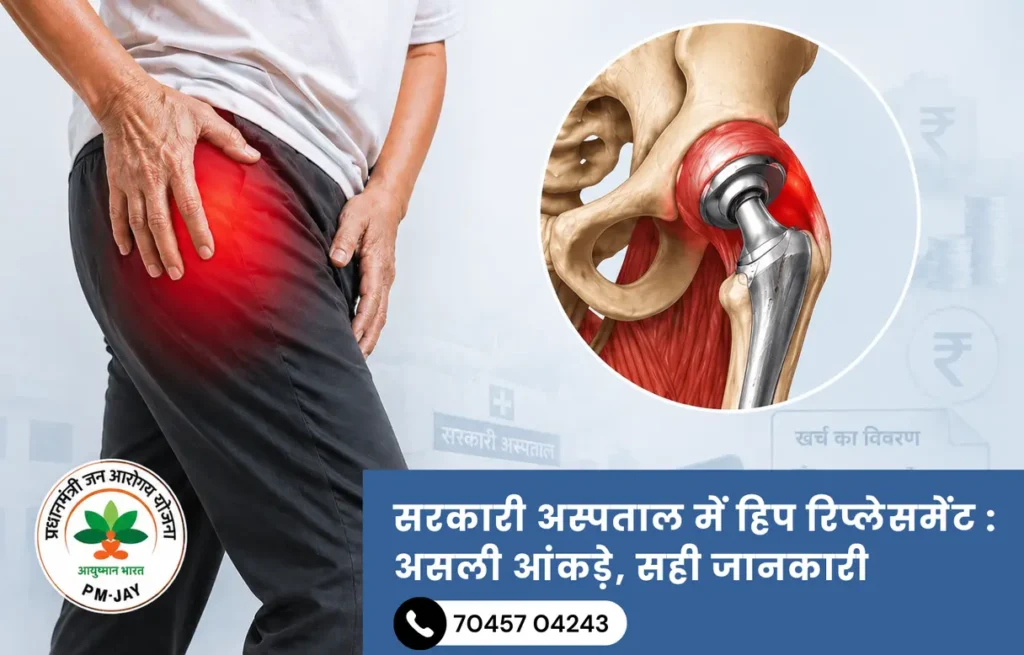
- Osteoarthritis – Gradual breakdown of cartilage inside the joint. Bones start rubbing against each other causing pain, stiffness, and swelling that builds slowly over months or years. Morning stiffness that eases with movement is a classic sign. This is the leading cause of knee replacement surgery in Indore.
- ACL or PCL Ligament Tears – The ligaments that stabilise the knee during rotation and direction changes. When these tear – usually during sport or sudden movements – patients describe a pop followed by immediate swelling and a feeling that the knee cannot be trusted. It will not heal on its own.
- Meniscus Tears – The C-shaped cartilage disc that cushions the joint. Twisting, deep squats under load, or sudden pivots can cause tears. Pain along the inner or outer knee edge, swelling over 24 to 48 hours, and a catching or locking sensation mid-movement are the typical signs.
- Rheumatoid Arthritis – An autoimmune condition where the body attacks its own joint lining. It tends to affect both knees at the same time, causes severe morning stiffness lasting over an hour, and comes with systemic symptoms like fatigue and body-wide aching. Needs rheumatological and orthopaedic management together.
- Patellar Tendinitis – Inflammation of the tendon just below the kneecap. Common in gym regulars, runners, and people who climb stairs heavily. Pain sits specifically below the kneecap and worsens with jumping, kneeling, or going downstairs.
- Bursitis – Inflammation of the small fluid-filled sacs that cushion the knee. Causes localised swelling and tenderness on the surface, often without deeper joint damage. Common in people who kneel frequently for work.
- IT Band Syndrome – Sharp burning pain on the outer knee that appears after running or cycling a certain distance. The iliotibial band gets irritated from repetitive friction. Almost never needs surgery – responds well to rest, stretching, and hip strengthening.
- Gout – Sudden, intensely painful flares from uric acid crystal buildup inside the joint. The knee becomes red, hot, and so tender it is difficult to bear any touch. Flares can settle in days but keep returning and cause progressive damage if the underlying problem is not treated. Commonly seen in Indore patients with diets high in red meat, organ meat, or alcohol.
Symptoms That Mean You Need a Knee Pain Doctor in Indore Today
Most knee pain can wait a few days for a proper appointment. These symptoms cannot. Get seen the same day if you have any of the following:
- Sudden severe swelling after an injury – could mean a fracture or complete ligament rupture
- Complete inability to put weight on the leg
- A visible change in the shape or alignment of the knee joint
- Fever combined with a hot, swollen knee – this can indicate septic arthritis, a serious infection that destroys the joint within days without treatment
- The knee has completely locked and cannot be moved in any direction
- Numbness or tingling in the foot or lower leg after a knee injury.
How Dr. Prince Uchadiya Diagnoses Knee Pain Before Any Treatment Starts
A rushed 10-minute consultation that ends in a prescription is one of the most common complaints patients bring to Dr. Prince Uchadiya after seeing other doctors in Indore. Good knee pain treatment starts with a proper diagnosis – and that takes time and a structured process.
Step 1 – Physical Examination
Before any scan is ordered, Dr. Prince does a thorough hands-on assessment. This includes testing range of motion, identifying exactly where the knee hurts when touched, running specific clinical tests to check ligament stability (like the Lachman test for the ACL and McMurray test for the meniscus), observing how the patient walks, and assessing surrounding muscle strength. For an experienced surgeon, this examination alone narrows down the diagnosis in most cases.
Step 2 – Targeted Imaging
An X-ray is the starting point – it shows bone structure, how much joint space remains, and whether bone spurs have formed. But X-rays cannot show soft tissue. When a ligament tear, meniscus injury, cartilage damage, or tendon problem is suspected, an MRI is the essential next step. Ultrasound is added when real-time imaging is more useful – particularly for bursitis, tendon tears, or fluid that needs draining.
Step 3 – Blood Tests When the Picture Points That Way
If rheumatoid arthritis, gout, or a joint infection is a possibility based on the examination, blood tests are ordered – ESR, CRP, uric acid, and rheumatoid factor. This step gets skipped in rushed consultations, which leads to patients being treated for mechanical arthritis when they actually have an autoimmune condition that needs a completely different approach.
Every Knee Pain Treatment Option Available in Indore – Ranked From Least to Most Invasive
Not every knee problem needs surgery. The majority of cases can be resolved or managed well without an operation – but only when the right treatment is applied consistently. Here is the full range of what is available:
1. Physiotherapy and Targeted Exercise
This is the most underused treatment in Indore and one of the most clinically effective. Most patients have either never done proper physiotherapy or gave up after two weeks because they expected instant results. A well-designed programme targeting the quadriceps, hamstrings, and hip abductors – done consistently over 8 to 12 weeks – can reduce knee pain as effectively as some surgical interventions in early to moderate arthritis.
The Mayo Clinic’s clinical guidance on knee pain specifically confirms this. The muscles around the knee are supposed to absorb load and protect the joint. When they are strong and working correctly, the mechanical stress on the cartilage drops significantly. Physiotherapy is not a fallback – it is a real treatment.
2. Weight Management
Every kilogram of body weight removed takes roughly 4 kg of force off the knee joint with each step. Over thousands of steps a day, that is a massive difference. A 5 to 10 percent reduction in body weight can reduce arthritis pain substantially and delay surgery by years. This is one of the highest-impact changes an overweight patient can make – and it costs nothing.
3. Anti-Inflammatory Medications
NSAIDs like ibuprofen, diclofenac, or etoricoxib manage short-term pain and inflammation. They are useful for acute flare-ups and allow patients to engage in physiotherapy more comfortably. They are not a long-term solution – prolonged unsupervised use carries real gastrointestinal and cardiovascular risks and should always be used under medical guidance.
4. Corticosteroid Injections
Injected directly into the knee joint, these bring inflammation down fast and provide relief that typically lasts 3 to 6 months. Works very well for rheumatoid flares, bursitis, and moderate osteoarthritis where inflammation is the dominant issue. Can be repeated at safe intervals. Does not reverse damage but creates a window where the patient can exercise, lose weight, and slow progression.
5. Hyaluronic Acid Injections
In a healthy knee, the joint fluid is thick and lubricating. In an arthritic knee, it thins out and loses that protective quality. Hyaluronic acid injections restore that lubrication. Results build gradually over 2 to 4 weeks and many patients get 6 to 12 months of improved comfort from a course of these. One of the best options for patients who are not ready for surgery or not yet at a stage where surgery is warranted.
6. PRP Therapy
PRP uses the patient’s own blood, processed to concentrate growth factors, which is then injected into the knee. These growth factors reduce inflammation and can stimulate some tissue repair. Works best for younger patients with moderate arthritis, tendinitis, and some meniscal injuries. Not a guaranteed fix for everyone, but a good proportion of patients get meaningful, sustained relief lasting 12 to 18 months. Low risk because it uses your own blood. Worth trying before committing to surgery.
7. Arthroscopy (Keyhole Surgery)
A tiny camera is inserted into the knee through small incisions. Dr. Prince can see the damage directly inside the joint and repair it – trimming or repairing a torn meniscus, removing loose fragments, smoothing damaged cartilage, or repairing ligament injuries – all without opening the knee. Most patients go home the same day. Walking resumes within days for straightforward procedures. Return to desk work is typically 1 to 2 weeks. Read more about arthroscopy surgery by Dr. Prince Uchadiya in Indore.
8. ACL Reconstruction
A torn ACL cannot repair itself. Left unaddressed, the knee stays unstable, the meniscus and cartilage take repeated damage from that instability, and early arthritis develops within 5 to 10 years. ACL reconstruction replaces the torn ligament using a graft taken from the patient’s own tissue, performed arthroscopically. Most patients walk without crutches within 2 to 3 weeks. Return to sport takes 9 to 12 months of proper rehabilitation – and that timeline cannot be skipped without significantly increasing re-injury risk.
9. Partial Knee Replacement
When arthritis has damaged only one compartment of the knee, only that section needs replacing. The healthy cartilage, bone, and cruciate ligaments are preserved. The result is a more natural-feeling knee, faster recovery, and better functional outcomes compared to total replacement for the right patient. Increasingly preferred for active patients with isolated compartment disease.
10. Total Knee Replacement
For severe, end-stage arthritis affecting all compartments of the knee where conservative treatment has genuinely been exhausted, total knee replacement is the most effective and durable long-term solution. Modern implants last 15 to 20 years. Most patients report dramatic pain relief. Walking with assistance starts within 24 hours of surgery, independent walking within a week, and full functional recovery takes 6 to 12 weeks. Dr. Prince performs this using computer-assisted techniques that improve implant accuracy, reduce blood loss, and shorten hospital stay.
Surgery vs No Surgery – How to Think About This Decision
No article can answer this for a specific patient without an examination and imaging review. But here is the framework Dr. Prince uses every day that may help you think through where you stand:
Surgery is likely not needed yet if:
- Pain started in the last 3 to 6 months
- Imaging shows mild to moderate changes without bone-on-bone contact
- A full physiotherapy programme has not been completed
- Swelling settles with medication
- Daily activities, while uncomfortable, are still possible
Surgery may be the right path if:
- Conservative treatment has been done properly for 3 to 6 months with no real improvement
- Imaging shows severe cartilage loss, a ruptured ligament, or a complete meniscus tear that cannot heal independently
- The knee gives way or locks during normal activity, making daily life unsafe
- Pain is consistently disturbing sleep or preventing basic mobility
- You are a younger active patient with an ACL tear and want to return to sport safely
How to Protect Your Knees Before Things Get Worse
The CDC’s guidance on osteoarthritis prevention points to weight management, physical activity, and injury prevention as the most evidence-backed strategies. None of them need a prescription. Here is what actually makes a difference:
- Lose weight if you are overweight – every kilogram matters enormously for knee longevity
- Strengthen your legs beyond just walking – targeted quad, glute, and hamstring exercises protect the joint in a way daily walking cannot
- Warm up before sport or gym – 5 to 10 minutes of dynamic movement before exercise cuts ligament and meniscus injury risk dramatically
- Reduce prolonged deep squatting and floor sitting – sustained extreme knee flexion accelerates cartilage wear over time
- Wear proper supportive footwear – flat rubber chappals shift load unevenly across the lower limb and quietly stress the knee joint with every step
- Check your Vitamin D and calcium – deficiencies are extremely common in Indore and directly affect bone and joint health
- Do not dismiss minor injuries – a sprained knee that “gets better” in a week may have developed internal instability that silently causes damage for years
Why Patients in Indore Trust Dr. Prince Uchadiya With Their Knees
There are plenty of orthopaedic doctors in Indore. What separates a good outcome from a poor one is not just the procedure – it is the clinical judgment behind every decision, the experience to recognise what is actually happening in a specific knee, and the integrity to recommend what is right for the patient rather than what is easiest to offer.
Dr. Prince Uchadiya is a Gold Medalist in Orthopaedics. He has performed over 2,500 successful surgeries across more than a decade of focused practice. He uses minimally invasive techniques wherever possible – smaller incisions, less tissue disruption, faster recovery. He recommends surgery only when it is genuinely the best available option. And every patient, whether they need an injection or a full knee replacement, is supported through the complete recovery journey including post-surgery rehabilitation at his Indore clinic.
Your knees carry you through everything. Getting the right care at the right time makes the difference between a knee that recovers completely and one that becomes a permanent limitation.