Roughly 80% of all adults will experience significant back pain at some point in their lives.
And when back pain becomes severe enough to push someone toward an MRI, a large portion of them walk out with a report saying “disc herniation” or “slipped disc.”
Then the panic sets in.
The word “herniated” sounds serious. It sounds surgical. People start worrying about paralysis, about never sitting properly again, about whether they need a major spine operation.
Most of that worry is unnecessary. Because here is the other number: approximately 90% of herniated disc patients do not need surgery at all.
But some do. And knowing the difference between those two groups is what this article is about.
If you are in Indore dealing with back pain, leg pain, sciatica, or a fresh MRI report with “disc herniation” written on it, read this before you do anything else.
What Is a Herniated Disc? The Real Explanation
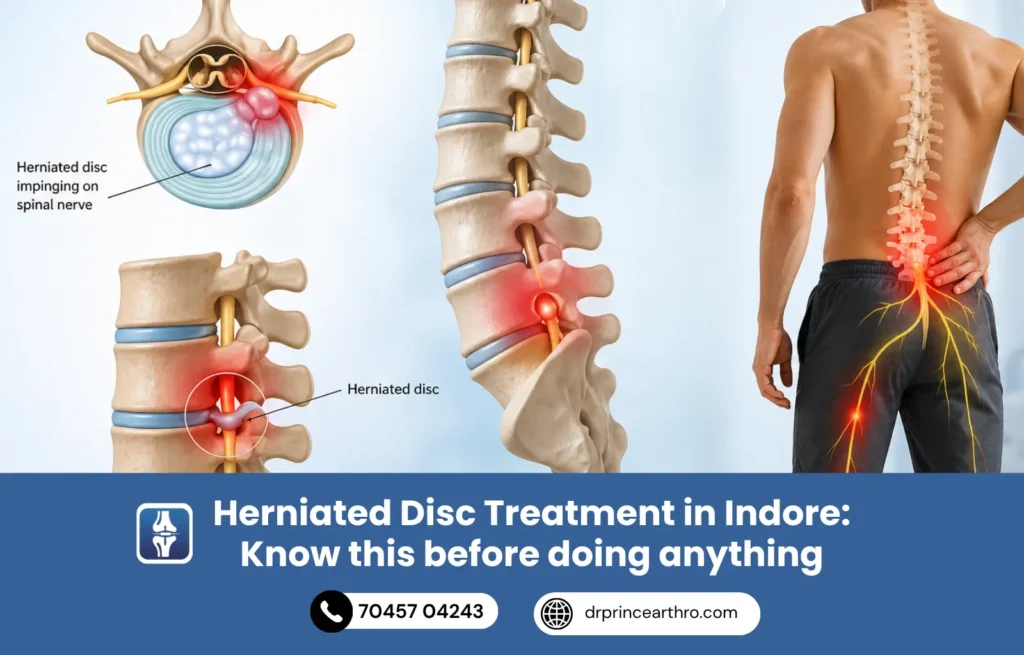
Your spine has 24 vertebrae stacked on top of each other. Between each pair of vertebrae sits a disc, a tough outer ring called the annulus fibrosus with a soft, gel-like center called the nucleus pulposus.
Think of it like a jam-filled doughnut. The doughnut casing is the annulus. The jam inside is the nucleus.
When the casing weakens or cracks, the jam inside can push outward. That is a herniation. Sometimes it bulges slightly (a disc bulge). Sometimes it pushes through completely (a true herniation or extrusion). When that displaced material presses on a spinal nerve root, that is when you feel the pain, numbness, tingling, or weakness in your leg or arm.
This is also called a slipped disc, though technically the disc does not actually slip anywhere. It deforms. The outer wall fails and the inner material migrates out.
It is not the same as a broken disc. It is not the same as a spinal fracture. And in most cases it is not a surgical emergency. If you have had a back injury or trauma and are worried about something more serious, you can read about fracture care and spinal trauma at our Nipania clinic separately.
Where Do Herniated Discs Actually Happen?
Not evenly across the spine. The data here is very specific.
According to research published in NCBI StatPearls, approximately 95% of lumbar disc herniations in people aged 25 to 55 occur at just two levels: L4-L5 and L5-S1.
These are the lowest two levels of your lower back, right above your tailbone. They bear the most weight. They are under the most mechanical stress. They degenerate faster than any other discs in the spine.
L4-L5 herniation typically compresses the L5 nerve root, causing pain and weakness along the outer calf and top of the foot.
L5-S1 herniation compresses the S1 nerve root, causing pain along the outer edge of the foot and sometimes reduced ankle reflexes.
Cervical (neck) disc herniations are the second most common, usually at C5-C6 or C6-C7, causing symptoms in the arm, hand, or fingers rather than the leg.
Knowing the level of your herniation helps you understand exactly which symptoms you should and should not be having. If your MRI says L4-L5 but your symptoms are in both legs and your bladder feels strange, that is a completely different situation from a one-sided leg pain. More on that shortly.
Herniated Disc Symptoms: What They Actually Feel Like
This is where most online articles stay generic. Let us be specific instead.
The typical herniated disc patient in Indore describes their experience in one of two ways:
The first group: sudden sharp back pain after lifting, twisting, or bending, followed days later by a shooting pain that runs from the lower back into the buttock, the back of the thigh, and sometimes all the way down to the foot. This is sciatica caused by nerve root compression. It is the most recognizable herniated disc symptom.
The second group: no clear injury, just a gradual worsening back pain over weeks or months, sometimes with occasional leg symptoms that come and go. These patients often have degenerative disc disease plus a herniation on top of it.
In both groups, the common symptoms include:
- Lower back pain, sometimes severe, sometimes a dull persistent ache
- Pain that radiates from the back into one leg (rarely both), following a specific pattern based on which nerve is compressed
- Numbness or tingling in the leg, foot, or toes
- Weakness when trying to lift the foot or stand on tiptoe
- Pain that gets worse with sitting, bending forward, or coughing
- Some relief lying flat with the knees bent
Pain that is worse sitting and better walking is a very characteristic herniated disc pattern. Pain that is worse walking but better sitting tends to suggest spinal stenosis instead, which is a different condition requiring its own evaluation.
Red Flag Symptoms: When a Herniated Disc Becomes an Emergency
This section is the most important one in the entire article. Most online resources on herniated disc treatment either skip this entirely or bury it at the bottom.
A small number of disc herniations cause a condition called cauda equina syndrome. This is when a large central disc herniation compresses multiple nerve roots simultaneously, affecting bowel and bladder control as well as sensation in the groin and inner thigh area.
Cauda equina syndrome is a medical emergency. It requires urgent surgical decompression, measured in hours, not days.
If you or anyone you know has back pain combined with any of the following symptoms, go to a hospital emergency department immediately:
- Sudden inability to control urination or defecation
- Numbness or tingling in the groin, inner thighs, or saddle area
- Weakness in both legs simultaneously
- Feeling that the bladder is not emptying fully
- Sudden sexual dysfunction alongside back pain
This is rare. The vast majority of people reading this do not have cauda equina syndrome. But it is important enough that every person with back pain should know these signs before assuming everything can wait for a Monday morning appointment.
What Your MRI Actually Means (And What It Does Not)
This is where a lot of unnecessary anxiety begins. Patients get their MRI, see words like “herniation,” “protrusion,” “annular tear,” or “foraminal narrowing” and immediately assume the worst.
Here are the facts that most clinics do not take time to explain:
A significant review of imaging studies found that disc bulges are visible on MRI in 30% of completely asymptomatic people in their 20s, and in up to 84% of asymptomatic people in their 80s. These people have no pain, no neurological symptoms, no functional problems. Their MRI just reflects normal age-related changes that happen to look concerning on a scan.
This is critical. It means an MRI that shows a herniated disc does not automatically explain your pain. And it means an MRI alone never drives the treatment decision. Your clinical symptoms, your neurological examination, and how the two correlate with the imaging finding together determine whether and how to treat.
A patient with severe sciatica, a positive straight leg raise test, and an MRI showing compression at L5 has a clear, consistent clinical picture. That warrants treatment.
A patient with mild back pain whose MRI shows a small disc bulge but whose examination is entirely normal may need reassurance more than intervention.
This distinction is exactly why seeing a specialist in Indore, not just a radiologist, matters for getting the right answer from your MRI report.
The 90% Rule: Who Does Not Need Surgery for a Herniated Disc?
The most reassuring thing to understand about herniated disc treatment is what science actually says about natural recovery.
According to a comprehensive review by the World Federation of Neurosurgical Societies, 60 to 90% of symptomatic herniated discs resolve spontaneously over weeks to months without surgical intervention. The disc material, particularly when it has extruded (fully come out) into the spinal canal, often gets reabsorbed by the body’s immune system over time.
The natural history of a herniated lumbar disc favors recovery. Most patients see meaningful symptom improvement within 6 to 12 weeks of conservative management.
Conservative treatment that works includes:
- Activity modification: Not complete bed rest, which is actually harmful for disc recovery. Staying mobile with careful activity restriction is the goal.
- Anti-inflammatory medications: NSAIDs reduce the inflammatory response around the compressed nerve root, which accounts for a significant portion of the pain.
- Physiotherapy: Specific exercises including McKenzie method techniques, core strengthening, and neural mobilization help reduce nerve sensitivity and restore movement. This is not generic gym exercise. It needs to be targeted and supervised.
- Epidural steroid injections: For patients with severe sciatica that is not responding to oral medication, an injection of corticosteroid around the compressed nerve root can reduce inflammation significantly and accelerate recovery. This is a common and effective option for many Indore patients who need faster relief.
- Heat and cold therapy: Useful for symptom management in the short term, particularly for muscle spasm around the affected level.
- Posture correction and ergonomic guidance: Many patients in Indore sit for hours at a desk or drive long distances. Simple postural changes can reduce daily loading on the herniated disc significantly.
The timeline for conservative treatment is typically 6 to 12 weeks of properly managed care. If symptoms are improving, even slowly, that trajectory should be continued. If symptoms are not improving or are worsening after 6 to 8 weeks, reassessment is needed.
When Surgery for a Herniated Disc in Indore Is Genuinely Needed
Surgery is not a shortcut. It is the right tool for specific situations. And when those situations are present, delaying surgery is the wrong call.
The indications for herniated disc surgery include:
- Cauda equina syndrome (emergency, as discussed above)
- Progressive motor weakness that is getting worse despite conservative care. If you are losing strength in your foot or leg week over week, that nerve is under excessive sustained pressure and needs decompression.
- Severe disabling pain that has not responded to 6 to 12 weeks of well-supervised conservative treatment
- A herniation that is causing documented neurological deficit on examination, corroborated by imaging
- The patient’s quality of life and ability to work or function are severely and persistently compromised despite adequate non-surgical management
What surgery is not indicated for: a painful MRI finding with no matching neurological symptoms. This is one of the most important clinical distinctions. Many patients in Indore come asking for surgery after seeing a dramatic-looking MRI, but if the clinical examination does not match the imaging findings, conservative management is almost always the better path.
Minimally Invasive Spine Surgery in Indore: What the Operation Involves
For patients who do need surgery, the modern approach is a far cry from the large open spine surgeries of twenty years ago.
The most common procedure for a single-level herniated disc is a microdiscectomy. This involves a small incision, typically 2 to 3 centimeters, at the level of the herniation. Using a microscope or endoscope, the surgeon identifies the compressed nerve root and carefully removes the herniated disc fragment that is pressing on it.
The disc itself is not removed entirely. Only the protruding fragment is taken out. The rest of the disc remains in place.
The procedure usually takes 45 to 60 minutes. It is done under general or spinal anesthesia. Most patients go home the same day or the following morning.
Leg pain relief after microdiscectomy is often immediate, because the nerve root decompression removes the source of the radicular pain. Back pain may take longer to settle, as the surrounding muscles and tissues need time to recover from the surgical approach.
For more complex cases involving multiple levels, instability, or associated spinal stenosis, more extensive procedures may be required. These cases are evaluated individually. We approach each surgical decision at our clinic in Indore the same way we approach every other joint and bone problem: conservatively first, surgically when the evidence supports it. You can learn more about our minimally invasive surgical approach through our arthroscopy and keyhole surgical techniques page.
Herniated Disc Recovery: What the Timeline Looks Like
Whether you are recovering conservatively or post-surgery, knowing what to expect at each stage removes a lot of stress.
Conservative Recovery (No Surgery)
Week 1 to 2: Acute pain management. Rest, ice or heat as needed, anti-inflammatories. Avoid positions that worsen leg pain. No complete bed rest.
Week 2 to 4: Physiotherapy begins. Neural mobilization, gentle core activation, posture work. Walking is encouraged.
Week 4 to 8: Progressive rehabilitation. Increasing activity. Most patients start feeling significantly better through this phase.
Week 8 to 12: Most patients return to normal daily activities. Return to work for desk-based jobs is usually possible within 4 to 6 weeks. Return to physical work depends on the role.
Month 3 to 6: Full recovery for most patients. Occasional residual tightness or mild pain is normal and continues to improve.
Post-Surgery Recovery (Microdiscectomy)
Day 1 to 3: Walking begins on the day of surgery or the next day. Pain from the surgery itself settles within a few days.
Week 1 to 2: Home rest, gentle walking. Avoid bending, lifting, or twisting.
Week 2 to 4: Physiotherapy starts. Focus on gentle movement, posture correction, early core activation.
Week 4 to 6: Most patients return to desk work. Driving resumes.
Month 2 to 3: Progressive return to physical activity under guidance.
Month 3 to 6: Full return to normal life for the majority of patients.
5 Myths About Slipped Disc Treatment That Patients in Indore Believe
These come up in the clinic almost every week. Time to address them directly.
Myth 1: “Rest completely for weeks, do not move at all.”
Wrong. Complete bed rest for more than two days actually slows disc recovery. Gentle, appropriate movement maintains disc nutrition and prevents muscle wasting. You should move carefully, not avoid movement entirely.
Myth 2: “If my MRI shows a herniation, I definitely need surgery.”
Wrong. MRI findings and symptoms do not always match. A herniation on MRI without corresponding neurological findings on examination rarely needs surgery. As discussed, up to 30% of completely asymptomatic people in their 20s have disc changes visible on MRI.
Myth 3: “Once a disc herniates, the problem is permanent.”
Largely wrong. Extruded disc material is actually absorbed by the body’s immune system over time. Studies show that larger, extruded herniations often show more spontaneous resorption than smaller contained bulges. Many patients with severe acute herniations make a complete recovery without any intervention.
Myth 4: “Spinal massage will fix a herniated disc.”
Massage can help with muscle spasm and pain around a herniated disc, but it does not address the structural problem. Aggressive spinal manipulation by an untrained practitioner on an acute herniation carries real risk of worsening the nerve compression. Physiotherapy based on assessed clinical findings is a very different thing from general massage.
Myth 5: “Surgery always fixes it permanently.”
Not always. Microdiscectomy has excellent success rates for leg pain relief, typically 80 to 90% at 5 years. But disc herniation can recur at the same level after surgery, and back pain (as opposed to leg pain) may persist in some patients regardless of surgical intervention. Surgery fixes the nerve compression. It does not reverse the underlying disc degeneration.
Exercises That Help Herniated Disc Recovery (And What to Avoid)
A good physiotherapist makes the difference between a smooth recovery and a prolonged one. Here are the principles that guide rehabilitation for herniated disc in Indore.
Movements that generally help in the acute phase:
- Prone lying (lying face down) to reduce disc pressure on the nerve
- McKenzie extension exercises, if they reduce leg pain centrally
- Gentle walking on flat ground
- Pelvic tilts lying flat to begin core activation
- Neural flossing techniques under physiotherapy supervision to reduce nerve sensitivity
What to avoid until cleared by your specialist:
- Forward bending under load (picking things up by bending at the waist)
- Prolonged sitting without lumbar support
- Heavy lifting
- High-impact activity (running, jumping)
- Twisting movements, especially under load
- Any movement that sends pain shooting down the leg, as this signals ongoing nerve irritation
How to Reduce the Risk of Another Herniated Disc After Recovery
A disc that has herniated once is more susceptible to future problems at the same level. The structural damage to the annulus fibrosus is real. But the disc can still serve you well for decades if you look after it.
- Build core strength consistently, year-round. The paraspinal muscles and abdominals are the disc’s external shock absorbers. Stronger core means less mechanical loading on the disc itself.
- Learn to lift correctly. Bend the knees, keep the back in a neutral curve, hold the load close to the body. This sounds basic because it is. And yet a significant portion of new disc herniations in Indore are caused by a single bad lift.
- Manage body weight. Each extra kilogram adds compressive force on the lumbar discs, particularly at L4-L5 and L5-S1 where herniations are most common.
- Break up prolonged sitting. The lumbar disc is under most pressure when seated. Long drives and desk work without breaks accelerate disc degeneration. Stand or walk for 5 minutes every 45 to 60 minutes if you sit for work.
- Smoking accelerates disc degeneration. The evidence on this is clear. Smoking reduces disc nutrition through microvascular changes, contributing to earlier and more severe degeneration. If you smoke and have a history of disc problems, quitting is one of the most evidence-based spine interventions available.
Why People in Indore Choose Dr. Prince Uchadiya for Herniated Disc Treatment
Getting the right assessment of a herniated disc requires someone who will spend time correlating your MRI with your actual examination findings, not just read a report and recommend surgery.
Dr. Prince Uchadiya is a gold medalist orthopedic surgeon trained at KEM Hospital, Mumbai, with over 10 years of clinical experience and more than 2,500 successful procedures. His clinical approach to back pain and herniated disc is conservative first, surgical when genuinely indicated, and always guided by what the patient’s long-term joint and spine health requires.
Patients from Vijay Nagar, Nipania, Palasia, Bengali Square, Mahalaxmi Nagar, and across Indore come to the clinic for second opinions, for MRI reviews, and for comprehensive back pain management that includes both non-surgical care and minimally invasive surgery when needed.
You can find more about our overall orthopedic services and approach at the Dr. Prince Uchadiya Orthopaedic And Joint Care Clinic homepage.
Dr. Prince Uchadiya’s Direct Take on Herniated Disc Treatment
The most common thing I see in patients who come in after being told they have a herniated disc is unnecessary fear. They arrive convinced they are heading for surgery, that they will be dependent on painkillers forever, or that their back will never be the same.
The first thing I do is sit with them and walk through their MRI with them, not as a radiological report, but as a map of what is happening in their spine. Most people have never had someone actually show them what their scan means. That conversation alone changes how they feel about the situation.
The second thing is the physical examination. I check nerve tension signs, reflexes, motor strength, and how your symptoms relate to specific movements. An MRI without an examination is just a picture. The examination is what tells you what the picture actually means for that person.
For the majority of patients, the plan is: structure your activity correctly, start proper physiotherapy, manage the inflammation, and give the disc time. I explain from the beginning that six to twelve weeks of good conservative management is a reasonable, evidence-based investment before considering anything more invasive.
For those who do need surgery, we do it efficiently, minimally invasively, and with a clear rehabilitation plan from day one. A good surgical outcome is not just about the procedure. It is about everything that happens in the weeks after it.
If you are sitting in Indore right now with back pain and a report that says “disc herniation,” come in. Get a proper assessment. You may need much less treatment than you think. Or you may need the right treatment quickly. Either way, you deserve to know which one is true for you.
10 Frequently Asked Questions About Herniated Disc Treatment in Indore
1. How do I know if my back pain is from a herniated disc?
The most characteristic sign is pain that radiates from the back into one leg, following a specific nerve pathway. This is called radiculopathy or sciatica. If you have back pain alone without any leg symptoms, a herniated disc is one of many possibilities and not necessarily the most likely. An MRI combined with a clinical examination gives the most accurate answer.
2. Can a herniated disc heal on its own without surgery?
Yes, in the majority of cases. Research shows that 60 to 90% of herniated disc patients recover without surgery when properly managed conservatively. The disc material is often reabsorbed by the body over weeks to months. Larger extruded herniations can sometimes show more resorption than smaller contained bulges.
3. How long does herniated disc recovery take without surgery?
Most patients experience meaningful improvement within 6 to 12 weeks of structured conservative management. Full recovery can take 3 to 6 months. Some patients have residual stiffness or mild discomfort that continues to improve beyond 6 months.
4. Is physiotherapy enough for a herniated disc?
For many patients, yes. Targeted physiotherapy combined with activity modification and anti-inflammatory management is the cornerstone of non-surgical herniated disc treatment. The quality of the physiotherapy program matters. Generic exercises are far less effective than a program tailored to your specific disc level and nerve compression pattern.
5. What does a herniated disc at L4-L5 or L5-S1 feel like?
L4-L5 herniation typically causes pain, weakness, or numbness along the outer calf and top of the foot. L5-S1 herniation causes symptoms along the outer foot, small toe, and sometimes reduced reflexes at the ankle. Many patients describe a sharp burning pain shooting down the back of the leg, classic sciatica.
6. What is the difference between a disc bulge and a disc herniation?
A disc bulge is when the outer annulus widens and pushes out evenly, without the inner nucleus breaking through. A herniation is when the inner nucleus pushes through a crack or weakness in the annulus. Both can press on nerve roots and cause symptoms. Herniations are generally more symptomatic, particularly when the disc material extrudes into the spinal canal.
7. When should I see a doctor urgently for a herniated disc?
Immediately, if you have loss of bladder or bowel control, numbness in the groin or inner thighs, or weakness in both legs at once. These are signs of cauda equina syndrome, which is a spinal emergency requiring surgery within hours. For other herniated disc symptoms without these red flags, an appointment within a few days to a week is appropriate.
8. What is a microdiscectomy and how long is the recovery?
A microdiscectomy is a minimally invasive surgery to remove the herniated disc fragment pressing on a nerve root. It involves a small incision, use of a microscope, and careful removal of only the displaced disc material. Most patients are walking the same day, return to desk work within 4 to 6 weeks, and to full activity within 3 to 4 months.
9. Will a herniated disc come back after surgery?
Recurrence is possible, though uncommon. Studies suggest a reherniation rate of approximately 5 to 10% after microdiscectomy. The risk is higher in the first few months post-surgery and is reduced by following rehabilitation guidelines, avoiding heavy lifting too early, and maintaining core strength long-term.
10. What is the cost of herniated disc treatment in Indore?
Conservative treatment costs including physiotherapy, medications, and imaging are significantly lower than surgical costs. For patients who require surgery, the cost varies based on the procedure type, whether one or multiple levels are involved, and hospital facilities. For an accurate assessment based on your specific MRI and clinical findings, a consultation with Dr. Prince Uchadiya at our Indore clinic is the best starting point.