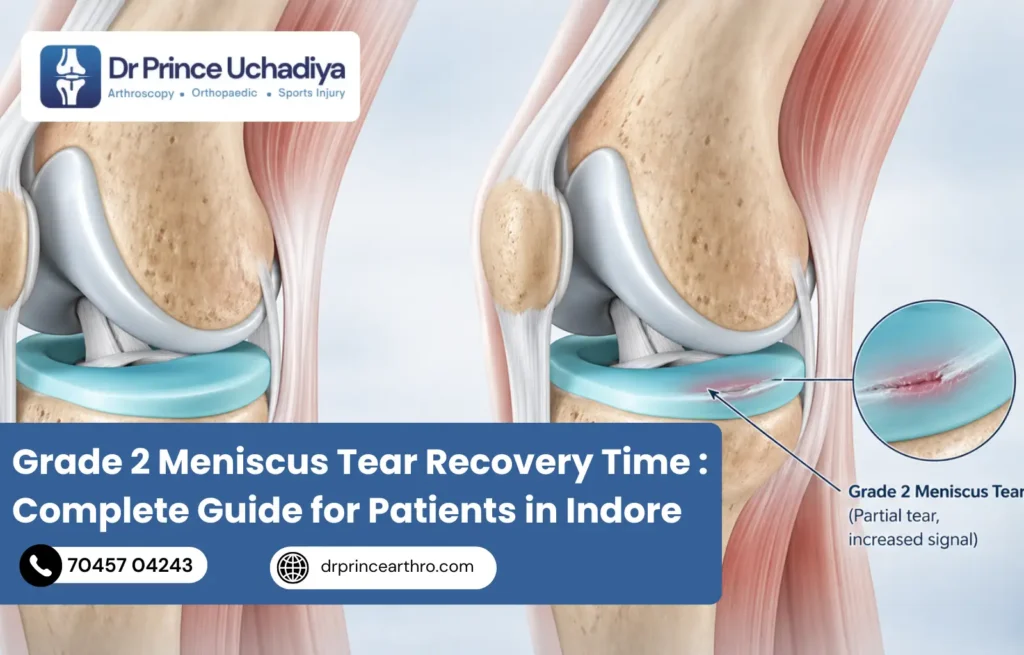
Your MRI report arrives, and somewhere in it you see the words:
Grade 2 signal intensity change in the posterior horn of the medial meniscus.
Most people read that and feel a knot in their stomach.
The next thing they search is: how long will this take to heal?
Will I need surgery?
Can I walk?
Can I go back to the gym?
The honest answer is that grade 2 meniscus tear recovery time is not a single fixed number. It depends on where the tear sits inside the meniscus, how old you are, how active you are, and whether your body responds to conservative treatment or eventually needs surgical help.
For most patients in Indore who come to us with a confirmed grade 2 tear, recovery without surgery typically takes 6 to 12 weeks. If surgery becomes necessary, full recovery generally extends to 3 to 4 months.
What Exactly Is a Grade 2 Meniscus Tear?
Before talking about recovery, it helps to understand what your MRI is actually telling you. The meniscus is a C-shaped piece of tough cartilage sitting between your thighbone and shinbone in each knee. You have two in every knee: one on the inner side (medial) and one on the outer side (lateral). Their job is to absorb shock, distribute weight, and stabilize the joint during movement.
When doctors classify a meniscus tear from an MRI, they use a grading system from 1 to 3:
- Grade 1: A small signal change inside the meniscus, but it does not reach the surface. Clinically mild, often asymptomatic.
- Grade 2: A more significant signal change that extends closer to the surface of the meniscus but does not break through it completely. This is a partial, internal tear. The meniscus is still structurally intact on the outside.
- Grade 3: The signal change extends all the way to the articular surface. This is a true complete tear that an arthroscope can directly visualize and probe. It is the grade most likely to require surgery.
The important point that many patients miss is this: a grade 2 finding on MRI does not automatically mean surgery. According to Cedars-Sinai Medical Center, grades 1 and 2 are not always considered surgically significant, and many patients with these grades can be managed without any procedure. What drives the treatment decision is not just the MRI grade but also your symptoms, your age, your activity level, and whether the tear is causing functional problems in daily life.
Why Grade 2 Tears Are More Complicated Than They Look
Not all grade 2 tears are the same. The location of the tear within the meniscus changes everything, including how likely it is to heal on its own.
Think of the meniscus as having three zones based on blood supply:
- The red-red zone: The outer third of the meniscus. This area has a good blood supply. Tears here have the best chance of healing without surgery.
- The red-white zone: The middle third. Reduced blood supply means slower, less predictable healing. Many grade 2 tears sit here.
- The white-white zone: The inner third. Virtually no blood supply. Tears here cannot heal on their own, and if symptomatic, they typically require surgical trimming.
A grade 2 tear in the red-red zone is a very different situation from a grade 2 tear in the white-white zone, even though both appear as grade 2 on your MRI report. This is why an MRI alone never tells the full story, and why a physical examination by an experienced orthopedic surgeon remains essential before any treatment plan is finalized.
Grade 2 Meniscus Tear Symptoms You Should Not Ignore
Grade 2 tears often produce symptoms that are present but not dramatic. People frequently walk into our clinic in Indore describing a nagging knee pain that came on after a twist or a fall, or slowly got worse over weeks without any specific injury. Here is what typically shows up:
- Pain along the inner or outer joint line of the knee, usually sharper when bending deeply or twisting
- Swelling that appears within hours to a day after the injury
- Stiffness, especially first thing in the morning or after sitting for a long time
- A feeling of tightness at the back of the knee when fully flexed
- Pain when climbing stairs or getting up from a low chair
- Occasional sensation of the knee “catching” but not fully locking
If your knee is fully locking (unable to straighten or bend completely), that is typically a grade 3 finding and needs urgent evaluation. A grade 2 tear rarely causes complete locking, but if you have any catching or instability during weight-bearing, you should not wait before seeing a specialist.
Grade 2 Meniscus Tear Recovery Time: The Week-by-Week Reality
These timelines are based on how our patients in Indore generally progress when they follow a structured plan. Your individual timeline may vary based on age, overall knee health, and how consistently you follow the protocol.
Week 1 to 2: Acute Phase (Reducing Pain and Swelling)
The first priority is bringing the inflammation down. Your knee is swollen, tender, and protective. This is your body doing its job. The treatment at this stage is straightforward but requires discipline:
- Rest the knee. Avoid activities that involve twisting, deep squatting, running, or prolonged standing.
- Apply ice packs for 15 to 20 minutes, three to four times a day. Do not place ice directly on skin.
- Wear a compression bandage or knee sleeve to minimize swelling.
- Keep the knee elevated when resting, above the level of your heart.
- Take anti-inflammatory medications as prescribed by your doctor.
A knee brace may be recommended depending on the tear pattern. In some cases, we advise patients to keep the knee in a slightly straightened position in a hinged brace for the first two weeks, especially when the tear is close to the red-white zone. This reduces stress on the tear site while it begins to stabilize.
At this stage, short walks on flat ground are usually fine. Avoid stairs unnecessarily. Crutches are rarely needed for isolated grade 2 tears but may be helpful if weight-bearing is significantly painful in the first few days.
Week 2 to 4: Early Rehabilitation Phase
Once acute swelling begins to reduce, the focus shifts to rebuilding the muscle support around the knee. A weakened quadriceps and hamstring group puts more stress on the meniscus during every step. This is why physiotherapy begins early.
Exercises at this stage are gentle and controlled:
- Straight leg raises to activate the quadriceps without bending the knee under load
- Heel slides to restore range of motion gradually
- Short arc quadriceps exercises
- Ankle pumps and calf raises to keep circulation moving
- Gentle cycling on a stationary bike with low resistance, if pain allows
Walking should feel more comfortable by the end of week 3 for most patients. Swelling should be noticeably less. If swelling is increasing rather than decreasing at this point, that is a signal that something needs to be reassessed.
Week 4 to 6: Progressive Loading Phase
This is the phase where patients in Indore often make the mistake of doing too much too soon. The knee starts feeling better, daily activities are manageable, and the temptation to return to sports or gym work is strong. This is precisely when re-injury risk is highest.
In weeks 4 to 6, the rehabilitation progresses to:
- Mini squats to 45 degrees, progressing to 60 degrees as tolerated
- Step-up exercises on a low platform
- Lateral band walks to strengthen hip abductors, which protect the knee
- Balance and proprioception exercises on a stable surface, then progressing to unstable surfaces
- Swimming is generally well tolerated at this stage
Most patients with a grade 2 tear managed conservatively can return to normal daily activities including moderate walking, light office work, and driving by the end of week 6, provided pain is minimal and swelling has resolved.
Week 6 to 12: Return to Activity Phase
By weeks 6 to 8, patients whose tears are healing well begin progressing to more demanding rehabilitation. This includes jogging on flat surfaces, full-depth squats under supervision, and functional movement patterns that simulate work or sporting demands.
A return to sport or physically demanding work typically happens between weeks 8 and 12 for a grade 2 tear managed without surgery. The decision should always be based on how the knee responds to progressive loading, not purely on the calendar date.
Before returning to any sport that involves twisting, cutting, or contact, we recommend a functional assessment. If the knee passes that assessment with no pain, no swelling, and full strength, return to activity is safe. If there is residual weakness or any doubt, the timeline is extended.
When Conservative Treatment Is Not Enough: Signs That Grade 2 Surgery May Be Needed
For many patients, a grade 2 meniscus tear heals with the approach described above. But not always. According to orthopedic research published in PMC (National Center for Biotechnology Information), if symptoms do not improve significantly after 6 to 8 weeks of well-supervised conservative treatment, surgical evaluation becomes appropriate.
The signs that suggest surgery may be necessary include:
- Pain that continues or worsens despite adequate rest and physiotherapy
- Persistent swelling that does not reduce with conservative care
- A catching or mechanical sensation in the knee that prevents normal movement
- Any locking of the knee, where it gets stuck in a bent or straightened position
- Complete inability to bear weight comfortably after 4 to 6 weeks of treatment
- Evidence on repeat MRI that the tear has worsened or become a grade 3
In these situations, arthroscopic surgery is the next step. For grade 2 tears, the surgical options are a partial meniscectomy (trimming the damaged tissue) or, in some cases where the tear is in a vascular zone and is suitable, a meniscal repair with sutures.
Meniscus Surgery in Indore: What the Procedure Involves
If conservative management has not worked and your surgeon recommends surgery, understanding the procedure removes a great deal of anxiety. At our clinic in Indore, we perform knee arthroscopy for meniscus treatment using minimally invasive techniques.
The procedure involves two to three very small incisions around the knee, each only a few millimeters wide. A tiny camera, the arthroscope, is inserted through one incision. This shows the inside of the knee on a high-definition monitor in real time. Surgical instruments go in through the other incisions.
Depending on what the surgeon sees, one of two things happens:
- Partial meniscectomy: The damaged portion of the meniscus is carefully trimmed away, leaving as much healthy tissue as possible. The goal is a smooth, stable meniscus that no longer catches or causes pain.
- Meniscal repair: If the tear is in the vascular red zone and is a good candidate, the surgeon places sutures to hold the torn edges together and allow them to heal. This preserves more meniscal tissue but requires a longer, more careful recovery.
The surgery typically takes 30 to 45 minutes. It is performed as a daycare procedure, meaning you go home the same day. Modern anesthesia techniques make it extremely comfortable.
Recovery After Grade 2 Meniscus Surgery in Indore
Post-surgical recovery timelines differ depending on which procedure was performed:
After Partial Meniscectomy
This is the faster recovery of the two options. Most patients can bear weight on the knee the same day or within 24 hours. Walking with minimal assistance is usually possible within a few days. Light daily activities resume within one to two weeks. Return to desk work typically happens within one to two weeks. Return to physically active work or sport happens at four to six weeks for most patients.
After Meniscal Repair
The recovery is deliberately slower because the repaired tissue needs time to knit together. Patients are typically on crutches with partial weight-bearing for four to six weeks. A hinged knee brace is worn during this period. Physiotherapy starts early but focuses on gentle range of motion without stressing the repair site. Full return to sport or heavy activity takes three to six months. The longer recovery is worth the effort because preserving the meniscus significantly reduces the long-term risk of knee osteoarthritis.
Exercises That Help Grade 2 Meniscus Tear Recovery (and Ones to Avoid)
One of the most common questions we get from patients across Indore is: what can I do at home to speed up recovery? Here is what helps and what to avoid.
Safe and Helpful
- Straight leg raises (lying flat, lifting the leg to 45 degrees)
- Seated knee extensions in the pain-free range
- Gentle heel slides on a smooth surface
- Stationary cycling with the seat set high to minimize knee flexion
- Swimming or pool walking once incisions are healed (post-surgery) or once acute swelling has reduced (conservative management)
- Hip strengthening exercises, particularly clamshells and side-lying leg raises
Avoid During Recovery
- Deep squats or lunges below 90 degrees of knee bend
- Any sport that involves pivoting, cutting, or lateral movement
- Running or jumping until cleared by your surgeon or physiotherapist
- Sitting cross-legged on the floor, especially in the early weeks
- Heavy lifting with the knees under load
Collaborating with a trained physiotherapist in Indore gives you a structured, supervised program that moves you through these phases safely. Dr. Prince Uchadiya works closely with rehabilitation specialists to ensure patients have a clear exercise plan at every stage of recovery.
How Age Affects Grade 2 Meniscus Tear Recovery Time
Age is one of the most significant factors in how quickly and how completely a grade 2 meniscus tear recovers. The meniscus has poor blood supply to begin with, and that supply diminishes further as you age. This affects the tissue’s capacity for self-repair.
Younger patients, generally below 40, tend to have more resilient meniscal tissue. Tears in the vascular zone have a reasonable chance of healing with conservative management. These patients also respond faster to physiotherapy and tolerate the loading phases of rehabilitation better.
Patients over 40 or 50 often present with tears that are partly degenerative rather than purely traumatic. These tears occur against a background of gradual cartilage wear and may coexist with early arthritis. Recovery is still very possible, but the timeline is longer and the likelihood of eventually needing surgical trimming is higher. As the Cleveland Clinic notes, degenerative meniscal tears in older adults can often be managed well without surgery, with realistic expectations about the pace of improvement.
Can a Grade 2 Meniscus Tear Heal Completely on Its Own?
This is the question every patient wants answered. The honest answer is: sometimes, yes. And sometimes, no.
Tears that are located in the red-red zone, are small, and occur in a younger person with no arthritis have a genuine chance of healing with rest and rehabilitation. The outer zone of the meniscus has a blood supply that can support tissue healing if the tear is protected adequately during the recovery period.
Tears in the red-white or white-white zone cannot heal on their own in a meaningful sense because the blood supply does not reach deep enough to drive tissue repair. These tears can become symptom-free if they are stable and do not mechanically interfere with knee function, but the structural tear remains on MRI.
This distinction matters practically. A patient may feel 100 percent fine after 12 weeks of physiotherapy, return to all activities, and never think about the knee again. Alternatively, a seemingly well-recovered knee may have episodes of pain return under high physical demand if the underlying tear was never fully addressed. This is why a follow-up appointment with your orthopedic surgeon is important even when things are going well.
Protecting Your Knee After Recovery: Long-Term Advice
Grade 2 meniscus tears leave the knee cartilage slightly more vulnerable than before, particularly if the tear was in the inner zones. Once you have recovered and returned to full activity, the following habits reduce the risk of re-injury and slow the wear on your knee cartilage:
- Maintain your quadriceps and hamstring strength year-round. Strong muscles are the best shock absorbers your knee has.
- Warm up before any physical activity with at least 5 to 10 minutes of light movement before loading the joint.
- Maintain a healthy body weight. Every kilogram of excess body weight places roughly four additional kilograms of force on the knee joint during walking.
- Avoid sudden increases in training volume. Gradual progression in any exercise program protects both menisci and cartilage.
- If you play sports, use proper technique, especially for landing, cutting, and pivoting movements that stress the meniscus.
- Never ignore a returning pain signal. If knee pain returns after a period of being symptom-free, have it evaluated early rather than pushing through it.
Why Patients in Indore Choose Dr. Prince Uchadiya for Meniscus Treatment
Choosing the right orthopedic surgeon for a meniscus tear is not just about technical skill. It is about getting an honest assessment of whether you actually need surgery or whether your knee can be managed conservatively, an assessment that serves your long-term knee health rather than defaulting to the operating room.
Dr. Prince Uchadiya is a gold medalist orthopedic surgeon with postgraduate training from KEM Hospital, Mumbai, one of India’s most respected orthopedic training programs. His subspecialty expertise includes arthroscopy, ligament reconstruction, and knee cartilage management. Patients from Vijay Nagar, Nipania, Palasia, Mahalaxmi Nagar, Bengali Square, and across Indore consult him both for conservative management plans and for surgical care when it becomes necessary.
You can learn more about the arthroscopic treatment approach at our clinic in Indore, or visit the Dr. Prince Uchadiya Orthopaedic And Joint Care Clinic homepage to book a consultation.
Dr. Prince Uchadiya’s Perspective: What He Tells Every Meniscus Patient
Every week, patients walk into the clinic holding an MRI report with “grade 2 meniscus tear” written on it, and the anxiety on their faces tells the story before they say a word. The first thing I tell them is this: your MRI is a piece of information, not a verdict. A grade 2 finding on imaging has to be read alongside what your knee is actually doing. I have seen patients with grade 2 MRI findings who had no meaningful symptoms at all. I have also seen patients with significant grade 2 tears who could barely walk. The MRI alone never makes the decision.
What I look for in the clinic is how the knee moves, whether there is joint line tenderness, whether you can load the limb, and whether the knee is stable. That physical examination tells me far more about how aggressively we need to treat this than any imaging alone.
My preference is always to exhaust conservative management first, properly supervised physiotherapy, activity modification, adequate time. Surgery is not a shortcut to faster recovery in most grade 2 cases. A partial meniscectomy, for example, gives you quicker relief but removes meniscal tissue that you cannot get back. Once that cushioning is gone, the cartilage underneath works harder over the years. So we think carefully before recommending surgery, and we only go that route when the clinical picture genuinely calls for it.
For active young people in Indore, whether you play badminton on weekends or walk long distances for work, the goal is always to get you back to what you love, safely, with a knee that can serve you well for decades. That means being honest about timelines, being disciplined about rehabilitation, and being willing to monitor the recovery rather than just waiting and hoping.
If you are reading this after receiving a grade 2 meniscus diagnosis, come in for a proper evaluation. The sooner you have a clear plan, the sooner recovery begins.
Frequently Asked Questions About Grade 2 Meniscus Tear Recovery
1. How long does a grade 2 meniscus tear take to heal without surgery?
Most grade 2 meniscus tears managed conservatively take 6 to 12 weeks to heal sufficiently for a return to normal activities. The exact timeline depends on the location of the tear within the meniscus, your age, and how well you follow your physiotherapy program. Tears in the outer vascular zone tend to heal faster than those deeper in the meniscus.
2. Can I walk normally with a grade 2 meniscus tear?
Yes, most patients can walk normally or near-normally with a grade 2 tear. Walking on flat ground is generally fine and is encouraged. What you should avoid in the early weeks is deep bending, twisting movements, running, or any activity that loads the knee under rotation.
3. Does a grade 2 meniscus tear always need surgery?
No. Grade 2 tears frequently heal or become symptom-free with conservative treatment including rest, physiotherapy, and activity modification. Surgery is considered only when symptoms persist beyond 6 to 8 weeks of proper non-surgical care, or when there are mechanical symptoms like locking or significant instability.
4. What is the difference between a grade 2 and grade 3 meniscus tear?
A grade 2 tear penetrates deeper into the meniscus than grade 1 but does not fully reach the articular surface. A grade 3 tear extends all the way to the surface and is classified as a true, complete tear. Grade 3 tears are more likely to cause locking and mechanical symptoms and are more frequently treated surgically.
5. Can physiotherapy alone heal a grade 2 meniscus tear?
Physiotherapy does not repair torn meniscal tissue at a structural level, but it plays a critical role in reducing pain, restoring range of motion, and rebuilding the muscle support that protects the meniscus. For many patients, this is enough to become fully functional and symptom-free. Some tears in the vascular zone may also undergo genuine tissue repair during this time.
6. How do I know if my grade 2 meniscus tear is getting better?
Signs of improvement include reducing swelling, decreasing pain with daily activities, improving ability to flex and extend the knee, and better tolerance of progressive exercise. If pain is increasing, swelling is worsening, or the knee starts locking or catching, those are signs that you need to see your orthopedic surgeon promptly.
7. Can I exercise with a grade 2 meniscus tear?
Specific exercises prescribed by a physiotherapist are not only safe but essential for recovery. General gym workouts involving deep squats, leg press with heavy load, running, or impact activities should be avoided until you are cleared by your surgeon or physiotherapist. Swimming and cycling are often well tolerated earlier in recovery.
8. What happens if a grade 2 meniscus tear is left untreated?
If a symptomatic grade 2 tear is ignored, it can progress to a larger, more complex tear. Ongoing mechanical stress on an unstable meniscus can also damage the articular cartilage underneath, accelerating joint degeneration and increasing the risk of developing osteoarthritis earlier than expected. Early treatment, even if it is conservative, is always better than delaying.
9. How much does meniscus surgery cost in Indore?
The cost of arthroscopic meniscus surgery in Indore varies based on the procedure required (repair versus partial meniscectomy), the hospital or clinic facility, and whether implants such as sutures or anchors are used. For an accurate estimate based on your specific MRI findings, a consultation with Dr. Prince Uchadiya at our clinic in Indore is the best starting point.
10. Is there any risk of the meniscus tear becoming permanent if I delay treatment?
Yes. A grade 2 tear that starts as a stable, manageable injury can progress to a complete grade 3 tear if the knee continues to be loaded without appropriate care. This is especially true for tears in the red-white or white-white zones where no blood supply assists healing. If conservative treatment is not started promptly, the window for non-surgical management may close, and a procedure that was once avoidable can become necessary. Seeking an evaluation early gives you the widest range of treatment choices.