Here is a situation a lot of people in Indore know all too well.
You go to bed fine. Sometime in the middle of the night, you roll onto your side and your hip lights up with pain. You shift positions. It helps a little. But the moment you get up in the morning and start walking, that dull ache on the outer side of your hip is already there, waiting for you.
Sound familiar?
That specific combination, outer hip pain, worse at night, worse lying on the affected side, worse after sitting then standing, is the calling card of trochanteric bursitis.
It is one of the most common causes of hip pain in adults, especially women. And it is also one of the most frequently dismissed, misdiagnosed, or left to drag on for months without the right treatment.
What Is Trochanteric Bursitis? Let Us Break It Down Simply
Your hip has small fluid-filled sacs called bursae. Their job is to cushion the friction between bones, muscles, and tendons as you move.
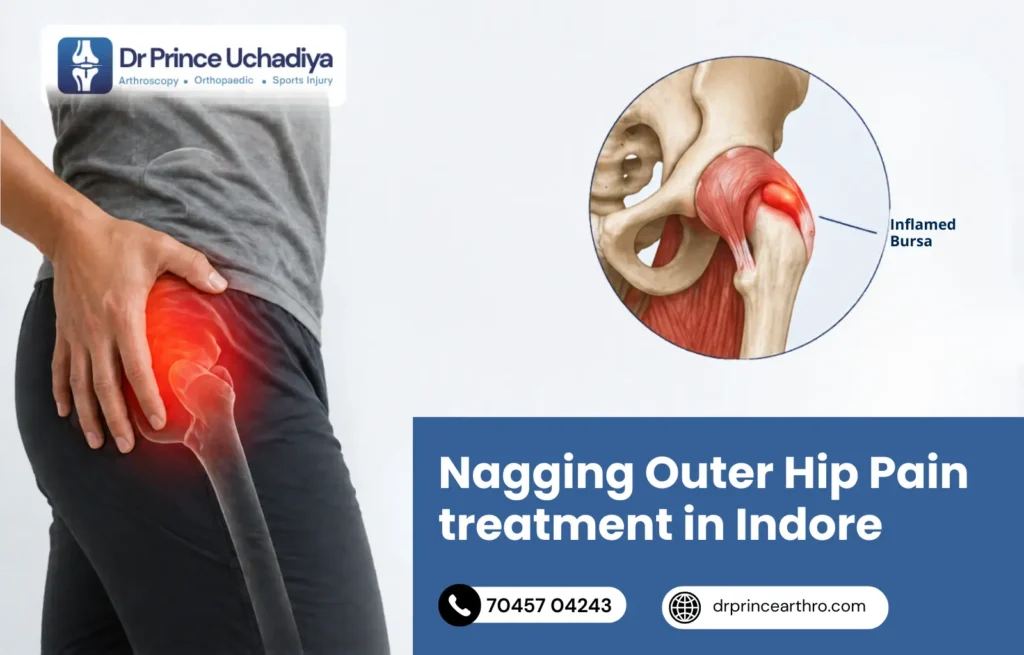
The greater trochanter is the bony point you can feel on the outer side of your upper thigh, where it meets the hip. There is a bursa sitting right there, protecting the tendons and the IT band as they glide over that bony prominence.
When that bursa gets irritated, inflamed, or overloaded, it swells. The swelling creates pressure. The pressure creates pain. That is trochanteric bursitis.
The medical world also calls this condition Greater Trochanteric Pain Syndrome (GTPS), because we now know the pain is not always purely from the bursa itself. The tendons of the gluteus medius and gluteus minimus muscles, which attach right there at the trochanter, often play a significant role in the pain too.
But the result is the same: a painful, tender, aching outer hip that can make sleeping, walking, climbing stairs, and basic daily life genuinely miserable.
How Common Is It? Here Are the Numbers
More common than most people realize.
Research shows trochanteric bursitis affects approximately 5 in every 1,000 adults.
And there is a strong gender pattern. It affects around 15% of women and about 8% of men across the general population. Women in their 40s to 60s are the most commonly affected group, though it is not exclusive to them at all.
Active adults who walk, run, cycle, or climb stairs regularly are also in the higher-risk group. So are people with tight IT bands, unequal leg lengths, spinal issues that affect gait, and those who have had previous hip injuries or surgeries.
Here is what is interesting: in a study of people with lower back pain, over 50% were found to also have GTPS when examined properly. The two conditions share a biomechanical relationship that is often missed when only one of them is being treated.
Trochanteric Bursitis Symptoms: What It Feels Like Day to Day
Let us go through the typical symptom picture, because recognizing it early makes the difference between a 4-week recovery and a 4-month one.
- Pain over the outer side of the hip, right at or around that bony point
- Pain that radiates down the outer thigh, sometimes reaching toward the knee
- Significant pain at night, especially when lying on the affected side
- Pain when getting up from a low chair after sitting for a while
- Discomfort when climbing stairs, walking uphill, or walking for long distances
- Tenderness to touch directly over the greater trochanter
- Pain that is sharp and intense at first, becoming a dull ache as the condition becomes chronic
- Occasional clicking or snapping sensation on the outer hip, sometimes with pain
One classic test that patients often describe to us at the clinic: if you can still put on your socks and shoes without major difficulty, that points more toward bursitis than hip joint arthritis. With true hip joint arthritis, that internal rotation required to dress the foot becomes very painful and restricted. With bursitis, the internal joint movement is usually preserved.
That small detail can be a useful home clue. But a proper clinical examination is still needed to be sure.
What Causes Trochanteric Bursitis? More Than Just Overuse
People assume bursitis is just something that happens when you exercise too much. But the causes are more varied than that.
Repetitive Friction
The iliotibial (IT) band, a thick strip of connective tissue running from the hip to the knee along the outer thigh, passes over the greater trochanter with every step you take. When the IT band is tight, it rubs harder against the bursa during walking and running, gradually irritating it into inflammation.
This is the most common mechanical cause, and it is why runners, cyclists, and people who climb a lot of stairs are particularly susceptible.
Direct Trauma or Fall
A fall onto the outer hip, a direct blow, or sleeping on a hard surface for extended periods can acutely inflame the bursa. This is common after road accidents and falls in older adults.
Leg Length Difference
Even a small difference in leg length changes the way you walk. The altered gait puts uneven load on the outer hip structures, causing the bursa on one side to take more friction than it should.
Spinal Problems
Conditions like scoliosis, lumbar disc problems, or lower back stiffness change how you walk and how you distribute load through the pelvis. This altered mechanics can create persistent irritation at the trochanteric bursa over time.
Gluteal Muscle Weakness
Weak gluteus medius and minimus muscles mean the IT band has to work harder to stabilize the pelvis during walking. More IT band tension means more pressure on the bursa underneath it.
This is why trochanteric bursitis is not just a local hip problem. It is often a whole-lower-limb biomechanical issue that happens to express itself at the outer hip.
Underlying Medical Conditions
Rheumatoid arthritis, gout, psoriatic arthritis, and calcium deposits in the tendons around the trochanter can all contribute to or trigger bursitis. In these cases, treating the underlying condition is part of the management plan.
Getting Diagnosed: What We Look For at the Clinic in Indore
The diagnosis of trochanteric bursitis is primarily clinical, which means a thorough physical examination is more informative than any single test.
During a consultation at our Indore clinic, we examine:
- The exact location of tenderness, whether it is right over the trochanter or more in the groin or deep joint
- Hip range of motion, to assess whether the internal joint is involved or pain-free
- The Ober test, which assesses IT band tightness
- The Trendelenburg test, which checks gluteus medius strength and whether there is hip drop during single-leg stance
- Response to direct palpation over the greater trochanter
Imaging is used to rule out other causes and to assess associated tendon pathology:
- X-ray rules out hip joint arthritis, calcium deposits, and bone lesions
- Ultrasound can directly visualize bursal swelling and detect gluteal tendon tears or thickening in real time
- MRI gives the most detailed picture of the bursa, tendon health, and surrounding soft tissue, and is used when the diagnosis is unclear or when conservative treatment has not worked
An important clinical note: a diagnostic injection of local anaesthetic into the bursa is also a powerful diagnostic tool. If the pain disappears within minutes of the injection, that confirms the bursa is the pain source. If it only partially helps, the tendons or other structures may also need attention.
Trochanteric Bursitis Treatment in Indore: Starting Conservative
Here is the good news. Most cases of trochanteric bursitis respond well to non-surgical treatment.
The key word is properly managed conservative treatment. Generic rest without addressing the underlying cause is not what we mean.
1. Activity Modification
Reduce or temporarily stop the activities that are loading the outer hip. This usually means cutting back on running, cycling, stair climbing, and prolonged walking while the bursa is acutely inflamed.
This does not mean complete rest. Gentle walking on flat ground is usually fine and preferable to bed rest.
2. Ice and Anti-Inflammatory Medication
Ice applied to the outer hip for 20 minutes, three to four times a day, reduces local inflammation. NSAIDs like ibuprofen or naproxen help manage pain and swelling during the acute phase.
Always take anti-inflammatory medication with food and consult a doctor before use if you have stomach, kidney, or heart concerns.
3. Physiotherapy
This is where the real work happens, and it is the most important part of long-term recovery.
A well-designed physiotherapy program for trochanteric bursitis focuses on:
- IT band stretching to reduce friction over the trochanter
- Gluteus medius and minimus strengthening to take load off the bursa
- Hip abductor and external rotator exercises to correct the mechanical imbalance
- Core and pelvic stability work
- Gait retraining if abnormal walking patterns are contributing
Research shows that a multimodal approach combining physiotherapy with other conservative measures allows 66% of patients to return to sports and 83% to return to labour-intensive occupations after approximately 3 months.
The patients who skip physiotherapy and rely only on injections or rest tend to see their pain return. The muscle weakness and IT band tightness that caused the problem in the first place are still there.
4. Corticosteroid Injection
When pain is severe enough to prevent sleep or daily activity, a corticosteroid injection directly into the trochanteric bursa is a highly effective short-term treatment.
According to Cleveland Clinic, corticosteroid injections can provide temporary to permanent relief for many patients with hip bursitis. Studies report response rates of 60% to 100% after one or more injections.
The injection is done in the clinic, takes only a few minutes, and is guided by anatomy or ultrasound for precision. Most patients feel meaningful relief within 48 to 72 hours.
One important point: injections manage the inflammation but do not fix the underlying cause. Without physiotherapy and activity correction alongside the injection, the bursitis is likely to come back.
5. Shockwave Therapy
Extracorporeal shockwave therapy (ESWT) is a non-invasive option that delivers acoustic waves to the outer hip, stimulating tissue healing and reducing pain.
Studies have shown it allows 64% to 76% of patients to return to normal physical activity, with minimal complications. It is particularly useful for patients who cannot tolerate corticosteroid injections or who have not responded to initial conservative care.
When Conservative Treatment Is Not Enough: Surgical Options
Surgery for trochanteric bursitis is genuinely rare. The vast majority of patients recover with the non-surgical approaches described above.
But when bursitis becomes chronic, when it has persisted for more than 6 months despite proper conservative management, and when imaging confirms significant bursal disease or associated gluteal tendon tears, surgical options become appropriate.
Bursectomy
The inflamed bursal sac is removed. This can now be done arthroscopically (keyhole surgery), which means small incisions, less pain, and faster recovery compared to open surgery.
Removing the bursa does not harm the hip. The hip functions normally without it, and a new bursa often forms over time in its place.
IT Band Release
When a tight IT band is causing persistent friction over the trochanter, a small portion of the IT band can be released surgically to reduce the tension. This is also done arthroscopically in most cases.
Gluteal Tendon Repair
When MRI shows significant tears of the gluteus medius or minimus tendons (sometimes called the “rotator cuff tears of the hip”), tendon repair surgery may be necessary. This is more involved than bursectomy alone and requires a more structured rehabilitation program afterward.
You can learn more about our approach to minimally invasive arthroscopic surgery at our Indore clinic, including what patients experience before and after the procedure.
Recovery Timeline: What to Expect at Each Stage
Whether you are recovering conservatively or post-surgery, here is a realistic picture of the timeline.
Conservative Recovery
Week 1 to 2: Acute pain management. Ice, rest from aggravating activities, anti-inflammatories. Gentle walking maintained.
Week 2 to 4: Physiotherapy begins. IT band stretching, gentle gluteal activation, posture work. Pain should be reducing noticeably.
Week 4 to 8: Progressive strengthening. Most patients see significant improvement by week 6 with consistent effort.
Week 8 to 12: Return to full activity for most patients. Athletes and those with physically demanding jobs may need a few extra weeks.
Post-Surgery Recovery (Arthroscopic Bursectomy)
Days 1 to 7: Crutches for comfort, gentle range-of-motion exercises begin almost immediately.
Week 1 to 3: Walking progressively. Pain from surgery settles quickly.
Week 3 to 6: Physiotherapy builds strength. Most daily activities resume.
Week 6 to 12: Return to sport and physical work for most patients.
5 Things That Make Trochanteric Bursitis Worse (That You Might Be Doing Without Realizing)
Here are the habits and patterns we see most commonly among patients in Indore that keep their bursitis dragging on longer than it should.
- Sleeping on the affected side without a pillow between the knees. This creates sustained compression on the inflamed bursa all night. Sleeping with a pillow between the knees in a side-lying position or switching to your back significantly reduces overnight irritation.
- Sitting with legs crossed or in a low chair. Both positions create IT band tension over the trochanter. Opt for chairs with firm, higher seats and keep the feet flat on the floor.
- Continuing to run or cycle through the pain. Moderate rest and activity modification during the acute phase is not weakness, it is smart management. Pushing through significantly extends recovery.
- Relying only on painkillers without physiotherapy. Pain relief without addressing the mechanical cause is like turning off the smoke alarm without putting out the fire.
- Getting one injection and assuming the problem is solved. The injection reduces inflammation. Without physiotherapy to correct the cause, the inflammation returns, usually within weeks to months.
Trochanteric Bursitis vs. Hip Arthritis: How to Tell the Difference
This is one of the most common diagnostic confusions, and it matters because the treatment is quite different.
With trochanteric bursitis: pain is on the outer side of the hip, tenderness is directly over the trochanter, internal hip rotation and movement are usually preserved, and you can still put on socks and shoes without major difficulty.
With hip joint arthritis: pain is deeper in the groin and often felt in the front of the hip, internal rotation and full bending of the hip are restricted and painful, the pain worsens significantly with walking distance over time, and putting on shoes and socks becomes genuinely difficult.
Both can coexist, which is why a proper clinical examination matters. Treating bursitis alone when arthritis is also present gives partial results at best.
Dr. Prince Uchadiya on Trochanteric Bursitis: What He Tells Every Patient
Trochanteric bursitis is one of those conditions where the gap between how straightforward it sounds and how much it disrupts people’s lives is enormous. Patients come in telling me they have not slept properly in weeks because of hip pain. Some have been managing it for months with painkillers alone and wondering why it keeps coming back.
The first thing I do is spend time on the examination. Bursitis sounds simple, but the outer hip has multiple structures, including the IT band, gluteal tendons, the hip joint itself, and the referred pain from the lower back, that can all produce overlapping symptoms. Getting the diagnosis right is the foundation of getting the treatment right.
For most patients, the plan is structured and evidence-based: reduce the acute inflammation, fix the mechanical cause through physiotherapy, and be honest about what activities need to change and for how long. An injection, when the pain is severe enough to prevent rehabilitation, is a valuable tool. But it is a bridge to physiotherapy, not a replacement for it.
The patients who do best are those who commit to the physiotherapy program even when the pain starts to ease. The temptation to stop early is real, but the hip abductor weakness and IT band tightness that caused the problem in the first place take weeks to properly correct.
Surgery is rarely needed, and I mean rarely. But when bursitis has been truly refractory for 6 months or more, with proper conservative care already tried, arthroscopic bursectomy is a very effective, low-risk procedure with a quick recovery. Nobody should be living with chronic outer hip pain indefinitely when good treatment options are available.
If you are in Indore with outer hip pain that has not improved in 2 weeks, or pain that wakes you at night regularly, come in. An accurate diagnosis changes everything.
10 Most Asked Questions About Trochanteric Bursitis
1. What does trochanteric bursitis feel like?
It typically feels like a sharp or dull ache on the outer side of the hip, right over the bony point where the thigh meets the hip. The pain often radiates down the outer thigh. It is worst at night when lying on the affected side and after sitting for long periods then standing. Learn more about our overall approach to hip pain at the Dr. Prince Uchadiya Orthopaedic And Joint Care Clinic homepage.
2. Can trochanteric bursitis heal on its own?
Mild cases can improve with rest and activity modification alone. But most cases, especially those persisting beyond 2 to 4 weeks, need structured physiotherapy to address the IT band tightness and gluteal weakness that are keeping the bursa irritated. Without treating the underlying cause, the bursitis tends to come back even if it settles temporarily.
3. How long does trochanteric bursitis take to heal?
With proper conservative management, most patients see significant improvement within 6 to 8 weeks. Full recovery, including return to all activities, typically takes 8 to 12 weeks. Chronic cases that have been present for months before treatment may take longer, sometimes 3 to 6 months of consistent rehabilitation.
4. Is it safe to walk with trochanteric bursitis?
Yes, gentle walking on flat ground is generally fine and better than complete rest. Avoid long distances, hills, and stairs during the acute phase. Running, cycling, and high-impact exercise should be paused until the inflammation has settled sufficiently.
5. Do I need a corticosteroid injection for hip bursitis?
Not necessarily. For mild to moderate cases, physiotherapy and activity modification are sufficient. Injections are most useful when pain is severe enough to prevent sleep or prevent participation in physiotherapy. They are a helpful tool, but they work best when combined with rehabilitation, not used alone.
6. What exercises help trochanteric bursitis?
The most effective exercises target the gluteus medius and minimus muscles and improve IT band flexibility. These include side-lying hip abductions, clamshells, wall-side hip abductions, and standing lateral band walks, along with IT band stretching in standing and supine positions. All exercise programs should be supervised by a physiotherapist initially, especially in the acute phase, to avoid aggravating the bursa. Our clinic works closely with physiotherapy specialists for exactly this reason.
7. Is trochanteric bursitis the same as a gluteal tendon tear?
No, but they are closely related. Gluteal tendon tears, sometimes called “rotator cuff tears of the hip,” involve actual structural damage to the gluteus medius or minimus tendons that attach at the greater trochanter. They can coexist with bursitis, and they produce very similar symptoms. Ultrasound or MRI is needed to distinguish between them, because the treatment for a significant tendon tear may include surgical repair rather than conservative care alone.
8. Can trochanteric bursitis affect both hips?
Yes, it can be bilateral, meaning it affects both sides. This is more common in people with gait abnormalities, leg length differences, or systemic inflammatory conditions like rheumatoid arthritis. Bilateral bursitis is important to recognize because it often points to a systemic or biomechanical factor that needs to be addressed, not just local hip treatment.
9. When should I consider surgery for trochanteric bursitis?
Surgery is considered when bursitis has been present for 6 months or more, has been properly treated conservatively including physiotherapy and at least one or two injections, and has not provided satisfactory relief. Arthroscopic bursectomy is the most common procedure, with low complication rates and a quick recovery. For patients with associated gluteal tendon tears, tendon repair surgery may also be appropriate. You can read more about how we approach arthroscopic procedures at our arthroscopy surgery page.
10. How is trochanteric bursitis different from hip arthritis?
The key difference lies in location and movement restriction. Trochanteric bursitis causes pain on the outer hip with preserved internal hip movement. Hip arthritis causes deep groin pain with restricted and painful internal rotation and bending. A simple home test: if you can still put on your shoes and socks without major pain, that points more toward bursitis than arthritis. But accurate diagnosis always requires a clinical examination. If you are unsure which you have, come in for a proper assessment at our Indore clinic and we will work it out together.